Symptoms
Addressing the symptoms of the UK’s healthcare staffing crisis seems like a never-ending vicious cycle. The shortage of permanent healthcare professionals in the NHS results in an increasing amount of stress for the existing workforce. It therefore comes as no surprise that retention and absenteeism rates have risen. The increase in these rates has a direct impact on the number of vacancies and consequently, on the quality of patient care.
A recent report from The King’s Trust states that 28% of nurses leave the NHS “within the first three years of their service” – and the number of doctors who leave the NHS is even greater. In 2017, the GMC reported that there were 9000 cases of ‘DREXIT’ (Doctor Exit) and 57.4% of F2 doctors chose not to progress into higher-training posts. There is a clear need for an increase in the numbers of doctors in training and in consultant positions – though with an increasing vacancy rate and a reduction in doctors choosing to continue training, how can we begin to rebuild the workforce?
Solutions
Remedium advocates for a ‘recruitment first’ approach. Increasing the number of health professionals in all grades and specialties is key in decreasing vacancies and therefore decreasing stress on the existing workforce, helping combat burnout and improve retention.
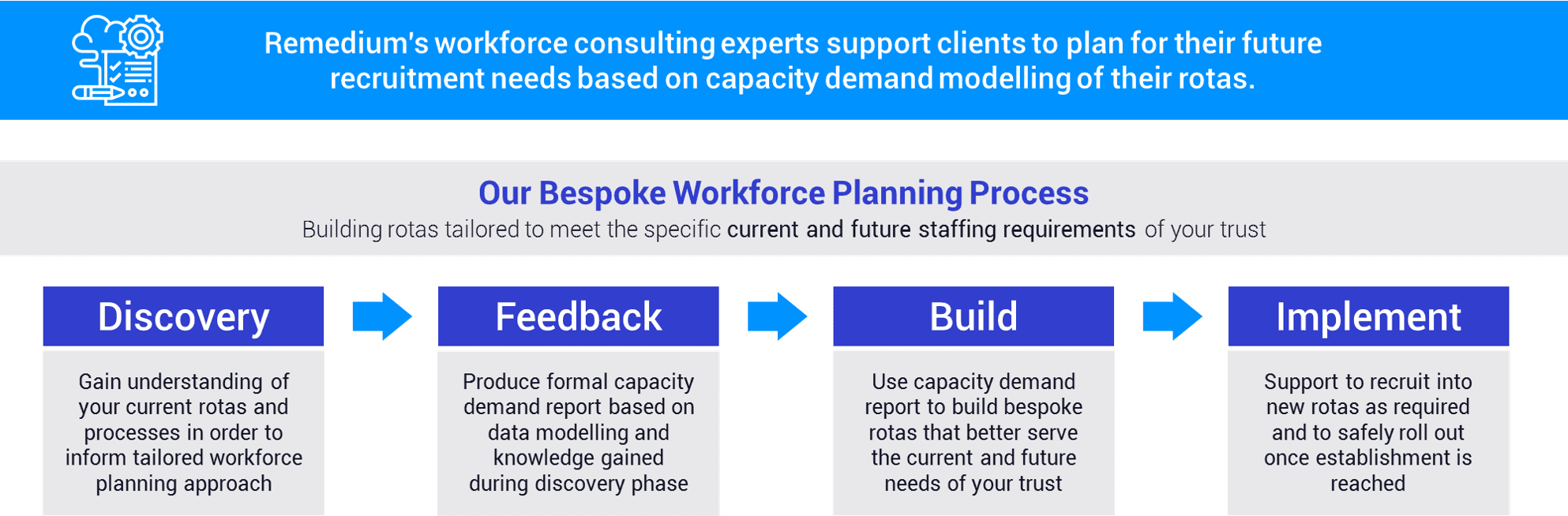
Remedium’s workforce consulting service provides Trusts with on-going support by using capacity demand modelling. Remedium begin by supporting Trusts with building a bespoke rota, followed by retention improvement processes.
At Remedium, we ensure that all doctors we recruit are supported at every step of their journey.
We promote a collaborative and inclusive work culture, which champions employees’ development and successes. We help connect clinicians with support networks, to:
-Foster lines of communication
-Improve diversity and integration
-Enable all health professionals to share and learn best practice.
Along with Remedium’s pioneering digital CPD accredited course, this integrated team-based approach is crucial in ensuring the smooth transition of international clinicians into their new role. An international doctor reiterated this by stating that when he started, he wishes that he had known “to not be afraid to ask for help.” His thought process was that:
“medicine is very hierarchical and you’re quite frightened of your seniors in some ways. Sometimes when you’re a junior you worry about asking for help. You think it’s a sign that you don’t know what you’re doing. In realiy, the opposite is true. You absolutely have to ask people to help. There are loads of situations where you particularly as a junior won’t know the answer. And the way that you learn and get better is to seek help.”
As international recruitment into the NHS is set to increase, the availability of support for internationally educated clinicians must also increase. Trusts often look to recruit UK trained clinicians – however, there are simply not enough UK-trained clinicians to fill the current vacancies.
References
https://www.kingsfund.org.uk/projects/positions/nhs-workforce




